E-Cigarette Summit: The Debate Goes On

“Much has changed since we ran the inaugural Summit in 2013, when calls for medicinal licensing and outright bans on e-cigarettes were dominant”.
Reading that in the introduction and welcoming statement in the e-cigarette summit programme highlights, at least in the UK, just how far things have come. When you have the likes of Professor Ann McNeill, Professor Robert West, Professor Linda Bauld, Professor Marcus Munafò, Dr Konstantinos Farsalinos, Professor John Britton, Professor Peter Hajek, Professor Ricardo Polosa talking about e-cigarettes folk sit up and listen. The list of names that gave talks is far longer. Including Clive Bates, Louise Ross, Lorien Jollye, Sarah Jakes, Professor David Abrams, Oliver Kershaw, Andy Morrison, the Department of Health represented by Alette Addison, Public Health England by Rosanna O’Connor.
The list of folks reads like an “A” list of proponents for e-cigarettes. My first thought when I saw the agenda was a big “wow”. Given that I’ve heard some of the names listed speak (mostly on video replay), it was definitely going to be a busy day. Really, the sheer amount of information presented over the day could easily have filled two days with a more relaxed pace with a lot more time for Q&A and discussions between delegates. It’s my only gripe about the day, alright there’s two, 0530 is a horrible time for a wake-up call.
Before I launch into the post proper, I just want to extend heartfelt thanks to Jessica Harding for giving me the opportunity to attend as a member of Vapers in Power, there were a lot of points made throughout the day that I simply would have missed by simply watching the #ecigsummit hashtag on Twitter. Onwards.
Professor Robert West
Much of Professor West’s talk focussed on the trends being monitored in smoking, cessation, NRT use and vaporiser use.
Professor West runs monthly surveys via the Smoking Toolkit Study (STS) which tracks the smoking and e-cig usage rates with representative samples of ~1800 participants since November 2006. Inclusion of e-cigarette use began in Q2 of 2011 where it has been made clear that the increasing use of vaporisers appears to be leading to a mirrored decrease in the use of “licensed products”. However, Prof. West did note that the decline of licensed products began before the inclusion of e-cigarettes.
Some interesting figures included that the use of any nicotine product (excluding tobacco) is around 25-30% among existing and former smokers. NRT use among never smokers is around 0.2% (this number may be down to error). Other interesting facts, the use of vaporisers across the entire age range is fairly stable (between 15-25% out of the 8,263 adults who smoke or who stopped in the past year, between 2013/14) with NRT more prevalent in the mid to upper age-ranges (35+).
Interestingly, the data suggests that there is a decline in the number of quit attempts. Is this the infamous “hardening” hypothesis at play or, as Prof West suggests, a blip? It is clear that successful attempts to stop smoking have risen since 2011 with vaporisers rapidly overtaking other NRT products as being the most popular, and seemingly most effective method.
As always, the information from the Smoking Toolkit Study is available from the Smoking in England website.
An interesting question from Clive Bates in response to the perception of harms of vaporisers (where current data suggests less than 50% think they are less harmful) was if it were possible to “increase granularity” of the responses, i.e. instead of asking “more or less harmful”, adding a degree such as “substantially less/more”. I do believe that ASH already has data on this from their YouGov surveys, but it would be interesting to see the inclusion of that in the STS.
Andrea Crossfield
Andrea is Chief Executive of Tobacco Free Futures, a social enterprise “tackling tobacco related health inequalities and poverty and ending children and young people’s exposure and addiction to tobacco”. Much like my visit to Harrow, Andrea focussed on her interactions with cessation practitioners and focus groups in conjunction with inclusion of vaporisers in the service.
Andrea ran a workshop in May to help develop guidance resources for smoking cessation practitioners. It seems that many of those that attended (~44) raised the usual concerns about renormalisation of smoking, efficacy, long-term health impact, tobacco industry involvement and the future of the stop smoking services role. Many of those present were cautiously positive if the product was “licensed”, had “evidence” or was “approved”. But the main aims were to try to reduce health inequalities in certain areas such as mental health and prisons.
Andrea did mention that there was no consensus among the participants of the workshop on whether vaporisers should be able to be prescribed but that around 80% of them were positive to promote vaporisers as a cessation aid. Additional commentary from that workshop included safety and licensing versus personalisation and choice.
According to Andrea, there is due to be some guidance documentation published by Public Health NW next week, which should prove to be an interesting read. It was interesting to hear more about the focus groups having considered the available evidence, yet still asking the question exactly what evidence is needed. The PHE Review went a long way to addressing many of the concerns and questions but this does need to be the foundation to be built on and reviewed regularly.
Professor Abrams commented “smokers having trouble quitting, may be more successful if the products were not viewed as a medication” when asking Andrea about inclusion of vaporisers in the SSS portfolio and how they were view by the users of the service. According to Andrea, many who used vaporisers felt “empowered” and some did continue to use the service.
It seems that the workshop was crucial in providing much-needed information towards educating practitioners about the benefits of vaporisers. More work like this is desperately needed.
Vaping in Enclosed Public Spaces: How can research inform regulation?
This was a double-act presentation with Marcus Munafò and Linda Bauld with specific focus on the use of vaporisers in enclosed public places and whether or not there is cause for concern.
Much of Marcus’s presentation focussed predominantly on the science of exhaled aerosol, the constituents of “room air” prior to use of vaporisers (and tobacco). In some of the studies mentioned, formaldehyde was already present before vaporiser use suggesting that some is exhaled by humans through metabolism. It was noted that there was indeed a spike in the levels of detected formaldehyde when smoking. It was made abundantly clear that although certain carcinogens can be detected at extremely low levels, it does not mean that they have any effect at a biological level. Especially when compared to the relative exposures from cigarette smoke. Marcus did point out that he “was exposed to more particulate matter walking here than from second-hand vaping”, which as you can imagine cracked a few smiles and laughs from the audience.
Interesting side-bar from Marcus, there does seem to be a need to introduce more nuanced policy to differentiate between tobacco and e-cigarettes. A comment that was later echoed by Linda.

Linda focussed more on policy than science, for which I was truly grateful as my head was spinning from the data shown by Marcus (so much so that I can’t read or understand my notes now). One of the arguments used by many opponents of vaporisers is the “renormalisation” and “undermining current smoke-free law”, both of which were simply quashed by Linda’s presentation. So far, to date there is little evidence to support either argument. A guidance document and questionnaire is due to be released by ASH and RSPH specifically for the smoke-free law compliance in relation to vaporisers.
The Chartered Institute of Environmental Health has issued statements not supportive of a blanket ban. Echoing Marcus, Linda highlighted a need for distinguishing separate policies and guidances for tobacco and vaping. The use of “passive vaping” as an argument, Linda says, is “no justification”. Though it is clear that the perceptions of the general public, such as the “looks like smoking” are often used to influence support (from the public, politicians and those within public health) for the usage restrictions in public places.
As the slide shows, Linda highlights the arguments being used to enforce public place restrictions yet hasn’t seen any conclusive data to support any of those statements.
ASH: E-Cigs and Children, what does the evidence tell us?
Deborah Arnott. According to the figures from ASH, use of vaporisers in never smokers remains low. Very low in fact. Below 1% of those surveyed (~2291). Rates of smoking in the 11-15 age range are declining (~25% in 2011) with similar rates being reported worldwide, except for Poland. There doesn’t seem to be any particular reason Poland is different, something which will no doubt be explored.
Arnott did re-iterate the point made by Linda in that there is currently no evidence of a “gateway effect” in the UK. ASH surveys are showing some experimentation (3% in 11 year olds) but almost zero regular use, even when regular use is framed as “used once monthly”.
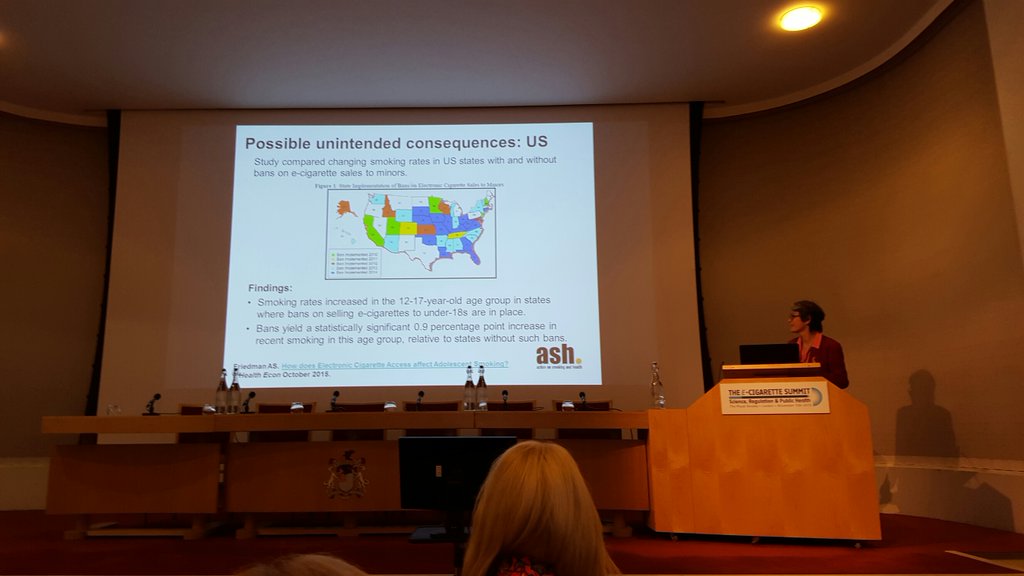
Going over to the US, Arnott highlighted where vaporiser bans were in effect and how, in those areas, smoking rates increased. This was based on a single study, so care should be taken. It was interesting to note that Arnott did mention that many studies are poorly reported, as in the headlines and media articles don’t tell the whole story, or that surveys don’t necessarily say what they actually say.
Unusually for Arnott, she did highlight potential unintended consequences are not considered when making regulations for vaporisers, something that she believes should be avoided, but she did make clear that where vaporiser use (between 2011 - 2014) has increased, cigarette use has decreased.
E-Cigs and the Challenge for Local Public Health Systems
As with many other speakers, this was the first time I’d heard Jim McManus speak and I listened in absolute awe. His talk covered a wide range of topics from a local health perspective. One of the key challenges that Jim notes is that a lot of bad science is being done, whether this is due to preconceptions or suspicions from the researchers (such as suspicions on renormalisation) isn’t particularly clear, but it did lead to this comment (thanks to James Dunworth for the inclusion of the quote on his review):
We are supposed to be an evidence based profession, so let’s put aside our misconceptions and start with the evidence . E-cig users are tax payers and have a right to expect a proper and unbiased service.
Jim went on to say that the position of his local health is based on evidence and reflection, but will be reviewed and updated regularly. This, I feel, is one of the key points that I took from the entire day. The evidence on e-cigs is mounting and constantly changing. That evidence needs regular review in order for any organisation to stay current. Systems and landscapes change, where do things fit and who should do what were two rhetorical questions Jim posed in his talk.
It is not the job of the Faculty of Public Health to “mark” scientific research of others
Jim’s public criticism of the responses to the PHE report were scathing, and as Clive Bates tweeted:
Just what we need in public health: tough, pragmatic, passionate and gritty… Jim McManus was brilliant
Some other key quotes from Jim:
Someone gives up smoking using an e-cigarette, should we not see this as a victory for public health?
The careful position taken by Public Health England convinces me more than increasingly shrill comments from some of those opposed to e-cigs.
Panel Q&A: Should e-cigarettes be prescribed to smokers?
The first panel Q&A session of the day was bound to be a lively one given how divisive this particular aspect is. This panel consisted of Deborah Arnott, Linda Bauld, Louise Ross, Andrea Crossfield, Peter Hajek and Jim McManus.
There did seem to be consensus that, to a point, an e-cigarette could be made available on prescription to increase the choice for those wishing to quit smoking, but it was clear that in a mixed economy, there shouldn’t be prescriptions for “prescriptions sake”, but to have a “prescribable” option. GP’s and primary should be able to deliver smoking cessation, but choice is paramount.
There were some comments on the current MHRA process not being streamlined, though (according to Arnott) one e-cig is “going through” but even she admitted that it is a challenge.
The comment from Peter Hajek on licensed products caught my attention, in that there is an inherent “danger” with licensing “squeezing” the market which will pose a significant policy and regulatory challenge.
Clive questioned the panel on how nicotine could be “reframed”, and that e-cigarettes have “nothing to do with the healthcare system”.
The end of the early morning session left me with a lot of thoughts. It is clear that the data isn’t supporting the “concerns” from the opponents to e-cigarettes and that educating the professionals to support smokers wishing to use them is essential. A good start on that has been made, but a lot more needs to be done. Sadly, I do get the sense that e-cigarettes are turning into a tool or weapon to be used against smokers. After all, the “endgame” as they like to phrase it, is to be “smoke free” by 2025. I do have a lot of concerns that anti-tobacco organisations, like ASH are on-board and it worries me that they, at some point down the line, turn on e-cigs. Time will tell.
An updated systematic review of the health effects of e-cigarettes
Charlotta Psinger. Admittedly, she did comment at one point “I’m one of the bad guys here”, which I believe is a good thing to have in such a scenario. In fact, I would have liked to have seen a lot more of the “bad guys” there, if only to give them the opportunity to digest what is being said in an open way. But I digress.
Charlotta started out by saying that there were 149 studies included in the review, each had “methodological challenges”. She highlighted a number of points on e-cig studies:
- Studies on adverse effects often had selection bias
- Human experiments included “naive volunteers” or utilised “short-term exposure”
- Animal studies often used “too much exposure” (formaldehyde anyone?)
- Misleading or missing information on ingredients
- Compared with smoking (26% of the studies reviewed were performed by the tobacco industry)
- Conflicts in “particle sizes”
Many studies on cytotoxic effects had conflicting results. Other studies had small sample sizes, insufficient exposure and/or short-term durations. Charlotta presented a large number of slides, but the highlights from her presentation included that harmful substances had been identified (though not necessarily at levels to have a biological effect). She did point out one example from Denmark, a national survey which contradicts the figures from the UK, where 81% of e-cigarette users still smoke. She drew similar references to Canada, US and Poland and questioned the health effects of dual use.
She did admit that there are probably health gains for “reluctant smokers”, and for users that quit smoking by using an e-cig. In conclusion, she highlighted that while e-cigs are “probably a safer product” than tobacco cigarettes, but would in effect change her views if persuaded by the evidence.
Theoritical health risks associated with e-cigarettes

Professor John Britton covered the theoretical risks of e-cigarettes, which I was keen to make a lot of notes on. Sadly, I didn’t.
He highlighted that there is an increasing risk of developing lung associated harms, even from e-cigarettes (usually in the form of COPD) as any carcinogenic particles would tend to accumulate at the “branch” of the airway into the lungs.
The devices being used by smokers, who have often been smoking for decades, have a high residual risk of cancer from smoking. Interestingly, while smokers and vapers have high risk, non-smokers also have an increasing risk of developing the same respiratory conditions, albeit at a much later point in their lives, and with a lower risk level.
The crux of his presentation, as Linda pointed out in her tweet, we cannot assume that low-risk is no risk. He did emphasise that the e-cig manufacturers must be prepared to face possible lawsuits in the future as some vaping ex-smokers may blame e-cigs should respiratory diseases occur. Vendors must therefore be prepared and able to show that they have done everything feasibly possible to ensure their products are as safe as possible.
Nicotine, is this a problem?
I’ve seen Professor Hajek give a talk before, but in this case he focussed on the “oh so evil” Nicotine. It was interesting to see the perceived harms from the public, Peter gave a further breakdown on e-cigarettes specifically (based on 2014 data):
- 18.9% believed e-cigs were equally harmful
- 20.1% believed e-cigs were more harmful
- 60.4% believe e-cigs were less harmful
- 20.6% “didn’t know”
It is actually incredibly depressing to see figures like that, given that 39% believe that e-cigs are as (or more) harmful than cigarettes. His view on the objectives of tobacco control were pretty damning.
- Fight the tobacco industry
- Eradicate nicotine use
- Prevent smoking related disease
He did point out in relation to point 3, quite forcefully, that tobacco control is not involved in relevant research or cessation and that the goal of preventing smoking related diseases can potentially undermine the first two objectives.
Nicotine, as we know, from tobacco, NRT and e-liquid is used by millions with fatal poisonings being extremely rare.
Professor Hajek also commented on the “addictiveness” of nicotine:
- Cigarettes highly addictive to non-smokers
- Difficult to get animals to self-administer nicotine (unlike alcohol, cocaine or heroin)
- NRT users & never-smokers are not becoming daily users
As mentioned by Deborah Arnott, Peter Hajek also mentioned how surveys are often mis-represented, especially with some of the “questions” asked and how certain organisations “classify” users:
- Ever Use = user
- Past 30 days = current user
- Smoker or current = daily user
E-cigarette users and current e-cigarette user are often implied to be one and the same even if only tried once. Hajek did state that dependence on e-cigs potentially very low, and that vigilance is needed.
E-Cigarettes and harm reversal
Quitting is the only way of removing the effects of 7,000 toxicants ~ Ricardo Polosa
Long term studies on the effects of e-cigarettes are still at least a decade away. Ricardo Polosa is researching the effects of e-cigarettes on smokers who have switched. By proving shifts in toxicology this translates to overall positives, and in his words harm reversal.
One study that Polosa discussed (Eclat) looked at the evidence for cessation rates of 300 smokers unwilling to quit that showed good success rates in terms of cessation and overall health benefits. Other studies mentioned blood pressure and how ex-smokers (now vapers) showed improvements in blood pressure levels.
Panel Q&A: How should the relative risks be communicated?
The second panel of the day focussed on communicating the relative risks between smoking and vaping and included Ricardo Polosa, Robert West, Charlotta Psinger, Penny Woods, Martin Dockrell and Sarah Jakes.
There was general consensus that clear and accurate information needs to be made available to smokers, vapers and the public at large. Declines in perceptions can often be attributed to “unscrupulous journalists” and that the headlines should be factually accurate. Sarah made the point that the Daily Mail is the primary source for many of the misleading headlines (in fact several headlines from the daily mail featured throughout the day on various slides). Sarah also pointed out that the information, while needing to be accurate, must also be understandable.
It was good to hear from Martin Dockrell on this question, he admits that PHE didn’t get it “100% right” but that they were “the first to do it”. Professor West noted that the “greatest clarity is when the speaking as a scientist or Public Health England” but care must be taken to avoid “tabloid language”. The “job is to communicate information as accurately as we can”.
Advertising rules & marketing after the TPD
As we expected, pretty much all forms of advertising will be banned once the TPD is implemented. Non-paid for blogs, tweets and some review videos will still be allowed as will sponsorship for UK only teams/events. While the UK Government is trying to be as hands-off as possible, there isn’t much wiggle-room on this aspect as it is clearly defined within the Directive. We were encouraged to join the list for more information on this issue.
The remit of the competent authority: MHRA
The Medicines and Healthcare products Regulatory Authority is a strange choice to regulate e-cigs as it doesn’t fall within their usual remit. Beryl Keeley from the MHRA took great pains to insist that the MHRA is aiming for the lightest touch possible, and see this as being underpinned by science and research. They plan to place much of the “burden of proof” on to the importers / vendors while they “simply” collect the data (though they will look at some, but not all of it).
There was some bad news though, it is confirmed that the limits on “liquid containers” such as tanks and cartridges will only be 2ml.
Retailers can expect to be charged for the privilege of using the notification system. The exact costings weren’t mentioned, but Beryl did say they would be proportionate and not as expensive as medical regulation. The MHRA do currently have a notification system (the “Yellow Card Portal”) which will be adapted for use in reporting to enable provisional actions such as product recall, though whether that would be the MHRA or Trading Standards would need to be decided. The concern there is that this portal could be used to report devices causing products being withdrawn because of user error or other “daftness”.
What is wrong (and right) with the TPD?
Following Beryl Keeley from the MHRA was Clive Bates. This was a presentation I was looking forward to. There wasn’t much “new” information contained in Clives presentation for those that follow his blog.
What is “right”?
- It’s not a ban
- It’s not medical
- It’s not the FDA
Clive discussed the foundations of the Totally Wicked legal challenge and how many of the principles and treaties were broken or ignored. There wasn’t a consultation, there is no justification, no impact assessments and little or no scrutiny by national parliaments.
Regulated too early because there was too much ignorance of the product
Common research misconceptions
I’ve been told that Dr Farsalinos can talk at length, but he is always worth listening to. Sadly, I didn’t make many notes on his presentation, but I did take away one quote:
Researchers cannot understand the differences between atomisers
A lot of the studies we have seen tend to either use old devices, or completely misunderstand what it is they are studying. He did discuss a study (which I believe is forthcoming) on the use of e-cigarette use (and smoking) changes and their effects on cessation rates. Many of his remarks on researchers that don’t understand the product seemed to, well, destroy Psinger’s discussion.
Panel Q&A: Implications of the TPD
When I read the synopsis of this panel, I really couldn’t wait. The implications of the TPD (when implemented) and how it would affect vapers, smokers and the general public. Included on the panel were Konstantinos Farsalinos, Clive Bates, Beryl Keeley, Robert Morrison, Andy Logan and Andy Morrison.
Andy Morrison kicked off proceedings with an impassioned speech which earned a well deserved applause. He stated that vaping saved his life and that these new regulations would force current vapers back to smoking or to the black market where safety could not be guaranteed and that “the TPD will kill people”. There was general consensus that the TPD is not the right regulatory approach to the innovative, disruptive products.
Evidence based consensus
Although Martin Dockrell was present, Rosanna O’Connor gave the presentation for Public Health England. There was in fact plenty to take from this presentation.
Roseanna made it clear that PHE were open to discussions from all parties on the available evidence, yet those opposing e-cigs declined to take part, and even declined the invitation to the Summit. Roseanna highlighted that PHE were working with Cancer Research UK on the E-Cigarette Research Forum to fully explore the emerging consensus and to carry on a useful and informed conversation with all interested parties.
The release of the PHE Review, commissioned by PHE proved to be the catalyst for a joint statement from a number of organisations and stakeholders.
The next steps for PHE are wide-ranging including addressing the use of e-cigs in public places, the e-cig symposium, NCSCT guidance, local policies and cessation advice (via the nine Public Health England centres across England).
Global approaches to regulating e-cigarettes
Ryan David Kennedy, the first of two speakers from Johns Hopkins Bloomberg School of Public Health covered the global approaches to regulating e-cigarettes. Which (in his own words) were a challenge to identify due to “localised issues”. Identifying 61 active policies at a country-wide level, the majority of them are using existing regulations via interpretation to apply them to e-cigarettes.
Identifying how policy makers fundamentally classified e-cigarettes:
- Imitative
- Derivative
- Substitutional

Prime example of existing rules being applied to e-cigarettes
The “Endgame” for Tobacco
Shirley Cramer from the Royal Society for Public Health. You’ll remember the “announcement” of a proposal to extend smoking bans into pub gardens but allowing e-cigs to be used. I’ll admit I had plenty of negative thoughts ahead of this particular presentation, though I tried to keep an open mind.
Public perception, of course featured highly in her talk, especially the perceptions of harmful ingredients:
- 87% think that Nicotine is the harmful component of cigarettes
- 48% think that caffeine is harmful
- 97% think that tar is the most harmful

Showing the “harm ladder” prompted a small sigh from yours truly, and a tweet from Sarah, but it also prompted a rhetorical question from Shirley:
- is fear of nicotine preventing uptake of e-cigarettes?
So she talked about an experiment where smokers were given “de-nicotinised” e-cigs. According to the results, this led to an 80% decrease in the number of cigarettes smoked, and an increase in the number of e-cigs vaped. This led to the conclusion that de-nicotinising cigarettes and forcing every shop to carry e-cigs would hasten the infamous “Endgame”.
My initial thought on that was “sacrifice one group in favour of another”, and one of the primary reasons I’m suspecting that e-cigs are being used more as a weapon against smokers, which I firmly disagree with.
Shirley did go on to say that safer forms of nicotine should be more accessible, and that an “outright ban on tobacco” is “unrealistic”.
What the science says about minimising harm and developing a consensus on methodology
The second speaker from the Johns Hopkins Bloomberg School of Public Health, Professor David Abrams gave a fascinating talk on the methodological flaws that are prevalent in many studies, and that the majority of these flaws, and interpretational flaws originate in ideology.
Let data not dogma speak

An interesting note from his discussion on the Markov model is the transitional phases. There is “no such thing” as one or the other, it’s simply a transition. Dual use is just that. A transition. Transitioning from being a smoker to being a vaper. Regardless of whether the user makes the switch over a short or long period of time, it is still a transition.
Citing data from the University of Michigan’s Monitoring The Future (MTF) survey, it is clear that the smoking rates within the US are falling, and have been steadily since 2010 but show a marked increase in decline between 2013 and 2014.
As with Dr Farsalinos and Deborah Arnott, Abrams highlighted that it is misleading to use flawed studies in a meta analysis, this only leads to compound errors. Including, but not limited to, poor exposure measures, selection bias, and a “blind approach”.
What was good, was the inclusion of Louise’s piece on scaremongering in relation to providing information to the public.
In closing, for the third or fourth time before Ann McNeill had to cut him off, he highlighted:
- Keep doing what we’re doing, and doom a generation
- Change the market, use non-combustible nicotine products to obsolete combustible market while minmising attraction to youth and non-users
In effect, let’s focus on tobacco, then we can look at whether or not nicotine is actually a problem.
Panel Q&A: How could the public health response to e-cigarettes better serve the public?
The final panel of the action packed day included David Abrams, Oliver Kershaw, Rosanna O’Connor, Lorien Jollye and Marcus Munafò covering, amongst other topics, communicating to the public, differentiating between tobacco control and public health, and finally personal choice.
Lorien opened the panel with the comment that the messaging surrounding nicotine must change and that e-cigs have been successful because they offer the user a choice and a sense of empowerment, we’ve done this ourselves without help. There was a sense that the general public viewed tobacco control and public health as a single entity (rightly or wrongly) and that there is “still a lot of confusion” from within public health.
That thought was echoed by Abrams who re-iterated his stance that science should not be clouded by ideology.
Final thoughts
The e-cigarette summit 2015 was an incredibly long, but completely worthwhile day. I am incredibly concerned about the role that tobacco control is trying to take in “leading the way” with e-cigs, it puts the image of the fox & scorpion in my mind, with tobacco control playing the scorpion. E-cigs were developed by the consumer and is being led by the consumer. As an innovative and disruptive product they have succeeded in encouraging the decline of tobacco smoking without any help from the state.
With such success, in the UK at least, thanks in large part to the “hands-off” attitude of the Government (for now at least), there does seem to be a lot of elements within tobacco control, and in certain corners of public health that are trying to impose their will on the direction that the product takes. To my mind, that isn’t necessary. But, it is useful when faced with such overwhelming opposition on a global scale to have the dedicated support from scientists, doctors, public health and tobacco control entities that have, by and large put their careers and livelihoods on the line to promote the product as an alternative to smoking.
On a personal note, I still firmly believe that all interested parties should attend events like this. Tobacco industry representatives, proponents and opponents of e-cigs, but for heaven’s sake, don’t forget us, the public. The users of e-cigarettes, the smokers and the dual users. All of us deserve to be heard and given the range of products to be able to make our own choices.